This brief review will bring to light some of the recent information concerning the relationship between silicone gel implants and Breast Implant Associated Illness up to the current date: 2019.

Breast implant surgery has been around for several decades and was the most common plastic surgical procedure in the US in 2017 with more than 300,000 patients having cosmetic breast augmentation. In addition about 100,00 breast reconstructions with implants are performed annually. Whether used for augmentation, replacement, or reconstruction, the majority of breast implants used in the U.S. and worldwide are silicone gel implants. Most women with silicone gel breast implants are satisfied with their result and their decision to have this procedure and do not suffer from associated illness. There is however, an ongoing controversial history regarding Breast silicone gel implant safety and especially more recently, textured implants with regard to implant associated illness . In the 1980s to 1990s, many thousands of women blamed silicone breast implants as a cause for many maladies including autoimmune disease and breast cancer. As a result in January 1992, the FDA issued a moratorium on the sale of silicone gel implants and only allowed saline implants for sale for first time cosmetic augmentation patients for the next 14 years. Soon thereafter Dow Corning, a prominent breast implant manufacturer filed for bankruptcy, in part due to massive legal liability despite prior evidence indicating that breast implants were not linked to any disease processes. In 1999 the Institute of Medicine (renamed National Academies’ Health and Medicine Division) independent experts concluded that though frequent complications from breast implants occur, there was no link to other medical conditions such as cancer, connective tissue disease, autoimmune disease, or other systemic illness. Simply put, these illnesses were “no more common in women with breast implant than in women without implants”. As a result the FDA advisory panel voted in a 5 to 4 decision, to allow silicone implants back on the market in 2006. This was a controversial decision and the Panel’s chairman, Dr. Whalen, in protest, resigned noting “To approve this device poses threats to women that are clearly unknown”. Debate continued and in November 2006 the FDA finally gave approval for silicone implants, made by Allergan and Mentor, to be made available in the U.S. for all appropriate patients over the age of 22 years old. It did so with the proviso that both companies were to conduct prospective large post implant approval studies over a 10 year period that included imaging surveillance, long-term safety issues including device-failure studies, as well as possible systemic harm due to silicone such as autoimmune and other disease processes. The FDA also warned that the risks of silicone gel implant complications are high and “you should assume the you will need to have additional surgeries”. Unfortunately, there was poor follow-up compliance in these study groups and after 2 years only 40% of Allergan subjects and after 3 years only about 20% of Mentor subjects remained in the study. It was on this basis of the available information, that I and other board certified plastic surgeons shared this limited available information with our patients; that though local complications can occur (rupture, capsular contracture, bleeding, numbness, etc) and that all breast implants whether silicone gel or saline would not last forever, most likely would have to be replaced and that they did not cause other disease processes.
Still, I and other plastic surgeons, over the years, would see increasing number of patients with ill defined problems and symptoms often involving connective tissue and autoimmune conditions that my patients and occasionally other medical doctors felt might be related to their silicone implants More recently, there is a growing body of evidence in the scientific literature linking silicone gel but not saline breast implants to autoimmune disease, and a growing number of Breast Implant Related Illnesses and symptoms. A systemic review of the literature was published in 2016 in Annals of Internal Medicine noting possible decreased risk for primary breast and endometrial caners but increase risk for lung cancer, rheumatoid arthritis, Sjogren syndrome, and Raynaud syndrome. However the authors concluded that the “evidence remained inconclusive about any association between silicone gel implants and long-term health outcomes. Better evidence is needed from existing large studies, which can be reanalyzed to clarify the strength of associations between silicone gel implants and health outcomes”. In the interim, after the FDA tightened reporting rules for enforcement in 2017, breast implant related conditions dramatically increased up to 20 fold. For example from less than 200 per year of possible breast implant related illness to greater than 8200 in the first half of 2018.
Still, an associated link to disease for silicone gel implants could not be made. This is because there was not enough cumulative data statistically analyzed to support the notion of “Breast implant Illness” until 2018. The post approval ten year FDA study of Silicone Gel and Saline implants was completed in 2016. This was the largest study of breast implant outcomes to date. MD Anderson Medical Center in 2018 reviewed the FDA study data of nearly 100,000 women with breast implants and published their findings in Annals of Surgery in the fall of 2018. They came to the following conclusions: Silicone gel implants but not Saline Implants are associated with Sjogren syndrome, Scleroderma, Rheumatoid Arthritis and Melanoma greater than double the general population risk. This supported the association in the literature review article in 2016. mentioned above. It should however be noted that despite this relationship, all are relatively uncommon processes. At about the same time, in October 2018, an article in the International Journal of Epidemiology was published titled “Silicone breast implants and the risk of autoimmune/rheumatic disorders: a real-world analysis”. This was a cross-sectional retrospective study in Israel analyzing computerized data, up to 20 years, and included nearly 25,000 silicone breast implant patients which they compared to nearly 99,000 matched women without implants. Their study demonstrated an association between silicone gel implants and the presence of autoimmune/rheumatic disorders. Of these, Sjogren’s syndrome, systemic sclerosis and sarcoidosis were most strongly associated with silicone gel implants. Other diagnoses such as fibromyalgia/chronic fatigue syndrome, hypo and hyperthyroidism, psoriasis, and being diagnosed with at least one autoimmune/rheumatic disorder was also noted to be more common in silicone gel implant patients regardless of reconstructive or cosmetic reasons for their silicone gel implants. Again, there was only a link to silicone gel implants and not saline implants. An important point of clarification needs to be made: these studies noted an association or correlation rather than causation. This means researchers found a relationship between different variables they were studying but and did not definitively conclude that the silicone gel implant was the definitive cause of these maladies, though this may be the case in the future pending and subsequent research studies. The American Society of Plastic Surgery (ASPS) and American Society for Aesthetic Plastic Surgery (ASAPS) have been closely monitoring adverse events associated with all types of breast implants. An ASAPS committee investigating this problem is finding a similar number of both saline and silicone implant patients have reported similar illness diagnosis and symptoms.* In interpreting this data one must take account of the moratorium on the use of silicone implants for 14 years (1992-2006) for aesthetic patients up until 2006. This means that approximately 4 million or more saline implant patients than silicone gel patients took place during this long time period. It is also likely that a time delay is present before symptoms or illnesses may be manifested. Therefore, if there was an equal likelihood for an illness to occur with both types of implants, theoretically there should be far greater saline associated illnesses than silicone. This is not the case. If in fact the number of these problems is similar, this infers there is a much greater likelihood that silicone gel implants have a higher associated incidence for these problems.
Perhaps the large scale study that may be most important and still needs to be done is to focus on those women with ruptured gel implants to answer the question if the risks of rare diseases would be even higher and prove causality. Unfortunately, this is a difficult study to do as few women follow the FDA guidelines to monitor their silicone implants with a MRI scan at 3 years then every two years (estimated at less than 10%) to make sure their implant is not ruptured. As a ruptured implant often does not cause symptoms (silent rupture) there maybe more than 150,000 women in the U.S. with ruptured implants and don’t know it. (assumes 2017 ASPS & ASAP statistics with 1% rupture rate per year and that most do not have MRI exams).
Recently, textured implants, both silicone and saline textured devices, have been found to be associated with late seroma, double capsule formation, and more importantly, a rare form of cancer called Breast Implant Associated Anaplastic Large Cell Lymphoma, BIA-ALCL. BIA-ALCL is a rare cancer, different from breast cancer, and usually curable with surgery. It is exclusively related to textured implants. Textured silicone gel implants are the most common round implant used in Europe, Central and South America and other regions and thought to have lower capsular contracture rates especially in subglandular position (above the muscle). All shaped silicone gel implants, for example, are textured. Reports of BIA-ALCL are from all companies in the USA though most cases to date are those made by Allergan and maybe related to their unique aggressive textured surface characteristics. As of this date there have been 615 identifies cases worldwide. Recently France banned Allergan’s Microcell and Biocell textured breast implants due to safety concerns and shortly afterwards in December 2018 Allergan stopped sale of their textured implants in the European Union. The exact incidence of BIA-ALCL is unknown until larger studies over a longer time line occur as there is a median of about 8 years post implant placement for ALCL to occur. In Australia for example, the incidence is somewhere between 1 in 1,000 to 1 in 10,000 but has been reported at a much lower rate than other countries. In the U.S. currently estimate at about 1:3800-1:30:000 but the incidence may increase with increased reporting and time. Note these only occur with textured primarily silicone gel implants and have not smooth silicone or saline implants. BIA-ALCL Symptoms may include breast enlargement, asymmetry, lump in breast or armpit, pain, overlying rash, breast hardening, or late larger fluid collection typically more than one year after implant placement. Diagnosis is made by analyzing the seroma fluid or by biopsy with specific CD30 immune staining tests. If positive a PET/CT scan is recommended to determine the extent of disease which will guide treatment. An oncologist will most likely be involved at this point. Fortunately, simply removing the implant and surrounding capsule (capsulectomy) is curative in most, but if BIA-ALCL is spread to lymph nodes or other body areas than chemotherapy is required. Post operatively, regular follow-up imaging studies for a few years to make sure there is no recurrence is typical but varies from case to case.
There are many myths being circulated in part by uninformed consumers, non-plastic surgeons and even plastic surgeons and medical societies that are misleading. Perhaps the most pervasive ones are that since the shell around saline implants are made of silicone, there is no additional risk or difference between a silicone gel or saline filled implant from your body’s standpoint. Further, a similar myth that since implants after 2006 are now cohesive and in particular highly “cohesive,” or “gummy bear” implants do not leak or rupture due to its semisolid nature, will last a lifetime and never need to be replaced. In reality, silicone gel even if cohesive is a mixture of silicone molecules of different lengths. The gel itself is sticky and adheres to the capsule. Short chain molecules (oils) can then migrate out of the gel with a broken shell. There is about 1-2% rupture rate per year of silicone gel implants including highly cohesive, “gummy bear” type in the first decade depending on the manufacturer then presumably a higher incidence after a decade.
Even without symptoms of breast implant related illnesses about 20% of women with silicone gel breast implants have them removed within a decade due to deflation, capsular contracture (distortion and hardening often with pain), fear, or other reasons. Silicone gel implant Deflation/Rupture at 8 years occurs between 7%-14% and Significant Capsular Contracture (Grade 3-4) ranges between 11-16% (FDA Core Trial Data) are most common reasons for removal.
So what are the safest and best options available?
These vary from person to person and it is best to discuss your goals and concerns with a board certified plastic surgeon by the American Society for Plastic Surgery experienced in both primary and revision breast cosmetic and reconstructive surgery. I will focus on some of the more common pragmatic choices that I provide to my patients which I feel is a combination of safety and overall minimizing the number of surgeries required during their lifespan. These are my personal biases and rationale for my recommendations from more than 30 years of practice. There is no singular right answer for everyone and I respect and acknowledge that other plastic surgeons will give alternative meaningful advice they feel are in their patients’ best interest with solid rationale based on their experience and individual research and reflection.
Implant Choice: If you wish to have an implant whether it is your first time, replacement, revision or coupled with other procedures such as a lift, reduction or augmentation I recommend the IDEAL Structured Implant® which is an engineered structured saline implant to feel like silicone but with safety profile of saline. As a FDA investigator for this implant, I have followed my patients for more than 9 years and have published and reported nationally on the comparison of this implant to silicone gel implants. To begin with IDEAL® implants have 3-6 times less deflation rate than silicone gel implants (2% at 8 years) and significantly lower capsular contracture rate than gel implants ( 6.5% vs 11-16%) while at the same time having the feel of silicone. It is not to be compared with, nor the same, as traditional saline implants which I do not prefer due to increased rippling and unnatural feel. IDEAL Implants® look and feel like silicone in my experience. IDEAL implant® monitoring is simple; just look in the mirror to see if your implant is intact rather than worry about silent rupture and the need, expense and hassle for repeated MRI scans. As the contents are only saline, it is absorbed. Since the shell is smooth, presently there is no risk for ALCL, nor are there any know associated risks with breast implant related illnesses which are to date only associated with silicone gel implants. Although I recommend to my patients with silicone gel implants that they should consider replacing their implants after 10-12 years (as rupture rates are relatively high) or whenever they are told they have a rupture, with IDEAL® implants there is no need to monitor or replace them unless there is a problem which will result in significantly less surgeries in their lifetime. When a silicone gel implant rupture occurs a longer and more expensive capsulectomy procedure is required, vs when simply replacement if an IDEAL implant® ruptures.
No Implant Choice: If you do not want to use an implant, wish to have yours removed but still wish to have increased breast volume, consider using your own fat to do the job. If you have sufficient fat in unwanted places, a fat transfer to the breast using your own tissue may be a good option for you. This has become so popular in my practice that we coined the term “California Breast Lift®” Patients are thrilled with removing unwanted fat, the perk of a smaller waist line & pants/shorts fitting slimmer and not having to worry about implant issues in the future. If you believe you are suffering from a breast implant related problem or illness and/or want your implants removed this may be a good option for you.
If your silicone gel implant is ruptured, an en bloc capsulectomy is customarily performed to remove as much of the silicone gel traces as possible. If you do not wish to use your own fat or have insufficient fat then simple removal, explantation with or without a capsulectomy, or lift (mastopexy), can be performed if desired. Your board certified plastic surgeon will guide you through this decision making process.
In summary, for the majority of women with or considering breast implant surgery whether it is for augmentation, replacement or removal, be aware of all of your options, potential risks and benefits of the procedure and search for the best and most experienced board certified plastic surgeon in your area. Let him or her know your concerns and be prepared to ask questions about risks, complications, and options to be fully informed. Although silicone gel implants seem to be associated with a number of illnesses and many complications, most women are spared and satisfied with their choice. Fortunately there are other options such as the IDEAL Structured Implant® and using your own fat (“natural breast augmentation,” California Breast Lift®) or simple removal (explanation) with or without a lift which can reduce or eliminate these concerns.
Larry S. Nichter, MD, MS, FACS
References:
- Balk EM, Earley A, Avendano EA, et al. Long-term health outcomes in women with silicone gel breast implants: a systematic review. Ann Intern Med. 2016;164:164–175.
- Coroneos CJ1, Selber JC, Offodile AC 2nd, Butler CE, Clemens MW. US FDA Breast Implant Postapproval Studies: Long-term Outcomes in 99,993 Patients. Ann Surg. 2019 Jan;269(1):30-36
- A. Watad, V. Rosenberg, S. Tiosano, J.W. Cohen Tervaert, Y. Yavne, Y. Shoenfeld, V. Shalev, G. Chodick, H. Amital. Silicone breast implants and the risk of autoimmune diseases: real world analysis. Int J Epidemiol. 2018 Dec 1;47(6):1846-1854
- Nichter LS, Hardesty RA, Anigian G: IDEAL IMPLANT® Structured Breast Implants: Core Study Results at 6 Years, Plastic and Reconstructive Surgery: 42 (1) 66-75, July 2018.

 An IDEAL Structured Breast IMPLANT® candidate is someone who likes the natural feel of silicone implants but also wants the benefits and peace of mind of a saline implant. The candidate should be over the age of 18 but not currently pregnant, breastfeeding, or with an active infection anywhere within the body. Patients with existing cancer or pre-cancer who have not received adequate treatment, as well as patients with bleeding disorders or poor overall health, may not be good candidates for the implants. Candidates for breast implants have a choice of 3 main incision sites which are underneath the fold of the breast, through the areola, or the armpit. The insertion site for the IDEAL Structured Breast IMPLANT® can be made in any of these places.
An IDEAL Structured Breast IMPLANT® candidate is someone who likes the natural feel of silicone implants but also wants the benefits and peace of mind of a saline implant. The candidate should be over the age of 18 but not currently pregnant, breastfeeding, or with an active infection anywhere within the body. Patients with existing cancer or pre-cancer who have not received adequate treatment, as well as patients with bleeding disorders or poor overall health, may not be good candidates for the implants. Candidates for breast implants have a choice of 3 main incision sites which are underneath the fold of the breast, through the areola, or the armpit. The insertion site for the IDEAL Structured Breast IMPLANT® can be made in any of these places.

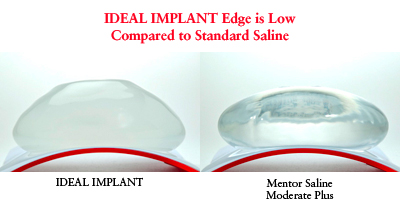 Natural feel is not the only thing women care about. The FDA approved intact silicone gel implants as safe. However, if a gel implant ruptures the implant and any gel should be removed including the surrounding capsule (capsulectomy). IDEAL® IMPLANT offers women natural feel without the risk of silent rupture. Women value the advantages of IDEAL® IMPLANT over silicone gel:
Natural feel is not the only thing women care about. The FDA approved intact silicone gel implants as safe. However, if a gel implant ruptures the implant and any gel should be removed including the surrounding capsule (capsulectomy). IDEAL® IMPLANT offers women natural feel without the risk of silent rupture. Women value the advantages of IDEAL® IMPLANT over silicone gel: Women wanting breast augmentation have until now faced a dilemma: a choice between safer but less natural-feeling saline implants, and more natural-feeling silicone implants which are perceived to come with health risks.
Women wanting breast augmentation have until now faced a dilemma: a choice between safer but less natural-feeling saline implants, and more natural-feeling silicone implants which are perceived to come with health risks. “The two-year clinical data from this study show that the Ideal Implant may provide a good alternative to current saline- or even silicone gel-filled implants. One of our most significant and unexpected findings was the low rate of capsular contracture for the investigational, double-lumen implant compared to current single-lumen saline implants.”
“The two-year clinical data from this study show that the Ideal Implant may provide a good alternative to current saline- or even silicone gel-filled implants. One of our most significant and unexpected findings was the low rate of capsular contracture for the investigational, double-lumen implant compared to current single-lumen saline implants.”


